Recovering from De Quervain’s tenosynovitis requires a balance between rest and functional movement. This guide explores essential recovery tips and explains how the 8080 Relief Patch for Thumb reduces tendon sheath irritation through targeted support, allowing you to stay active while accelerating your natural healing process.
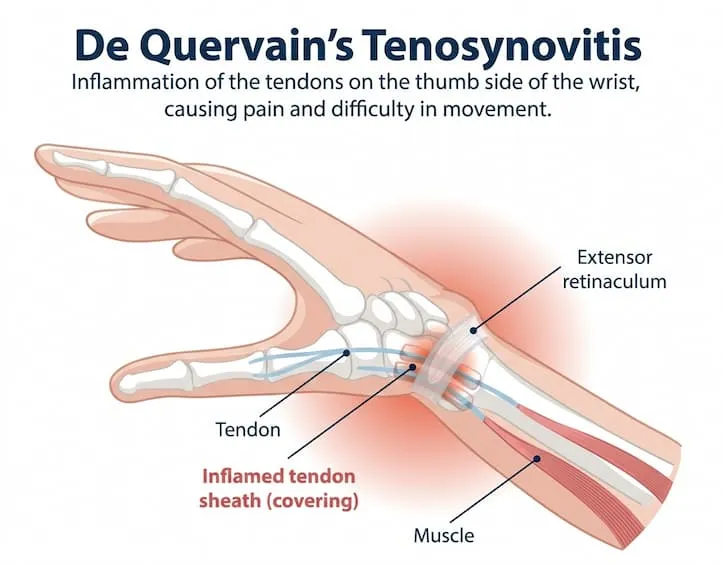
Tenosynovitis refers to inflammation of the tendon sheath, the protective layer that surrounds certain tendons, especially in areas where tendons pass through narrow spaces.
In contrast, tendinitis involves inflammation of the tendon itself. Although the two terms are often used interchangeably, they affect different anatomical structures. This distinction becomes especially important when symptoms are persistent or repeatedly aggravated by daily activities.
A tendon is a strong fibrous tissue that connects muscle to bone and transmits force to produce movement. A tendon sheath is a thin, fluid-filled structure that surrounds some tendons, allowing them to glide smoothly during repetitive motion while minimizing friction. When this gliding system is disrupted, pain and movement limitations can occur—even without direct structural damage to the tendon itself.
The type most commonly affecting the thumb is De Quervain’s tenosynovitis, a condition involving inflammation of the tendon sheath at the base of the thumb. It affects two thumb tendons—the abductor pollicis longus (APL) and extensor pollicis brevis (EPB)—as they pass through a tight sheath near the thumb base. Repetitive actions such as gripping, texting, lifting, or frequent smartphone use can irritate this area, leading to pain, swelling, and difficulty moving the thumb. This is why many cases described as “thumb tendinitis” are actually tenosynovitis, and often require more than rest alone.

Tenosynovitis may improve on its own in some cases, particularly when inflammation is mild and addressed early. However, because the condition involves the tendon sheath, recovery often depends on how effectively friction and repeated irritation are reduced during daily activities. For some individuals, symptoms improve within a few weeks. For others, recovery may take longer if mechanical stress on the tendon continues.
Continued use without adequate rest can maintain or worsen inflammation within the tendon sheath. As swelling increases, the internal space of the sheath becomes more restricted, leading to increased friction during movement.
Over time, this may result in:
Without appropriate management, tenosynovitis can become chronic and recurrent, potentially prolonging recovery time.
Tenosynovitis may require further attention when:
These signs may indicate ongoing mechanical irritation, significant sheath thickening, or the need for additional support and targeted management rather than rest alone.
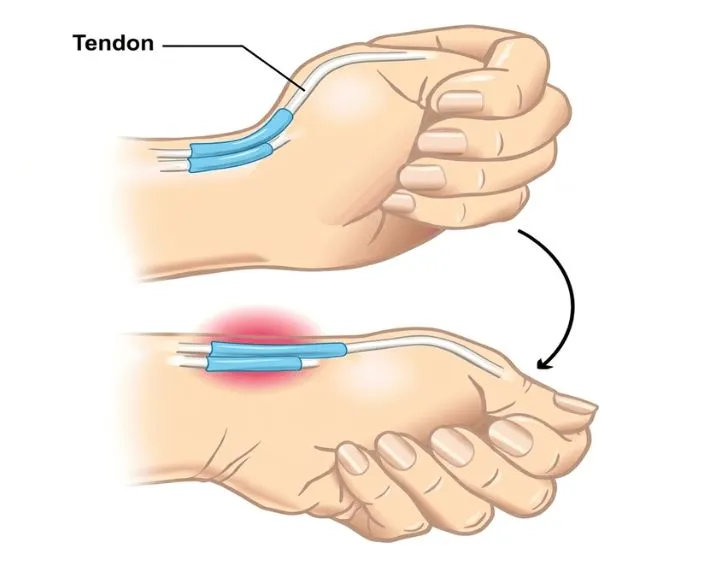
When tenosynovitis occurs, people often try stretching, massage, or heat to relieve pain. However, these approaches are not always appropriate, as tenosynovitis involves inflammation of the tendon sheath, where excessive movement or increased circulation may worsen irritation. Choosing the right approach at the right time is important to avoid prolonging symptoms.
Stretching is generally not recommended during the acute stage, when pain, swelling, or tenderness is present. Stretching can increase friction between the tendon and its sheath, potentially aggravating inflammation.
Gentle stretching may be considered only after pain and swelling have clearly improved, and should always be performed within a comfortable range—without forcing movement.
Heat therapy should be avoided when tenosynovitis is actively inflamed, especially if there is visible swelling or warmth around the affected area. Heat increases blood flow, which may contribute to additional tissue swelling and make tendon gliding more difficult.
Heat may be more appropriate in later stages, when stiffness remains but signs of active inflammation have largely resolved.
Massage may help relieve tension in surrounding muscles. However, direct massage over an inflamed tendon sheath is usually not advised, particularly in the early stages. Deep or aggressive massage can increase irritation and delay recovery.
If massage is used, it should be gentle and focused on nearby muscles rather than directly on the painful area, and only when acute symptoms have settled.

Taping is commonly used as a conservative approach for tenosynovitis, especially when symptoms are related to repetitive use. Rather than treating inflammation directly, taping works by modifying movement patterns and mechanical stress. This may help reduce ongoing irritation of the tendon sheath.
Taping helps manage tenosynovitis by guiding joint movement and reducing mechanical irritation to the inflamed tendon sheath. By limiting excessive or repetitive motion, taping alters the way force is transmitted through the tendon and reduces friction within the sheath.
As a result, taping can help:
Its effects are mainly supportive and short-term, making taping most useful during specific activities that would otherwise trigger symptoms.
The 8080 Relief Patch for Thumb serves a supportive and movement-guiding role in managing tenosynovitis, particularly thumb-related conditions such as De Quervain’s tenosynovitis.
It is designed for individuals who experience pain, weakness, or discomfort during daily hand use and require targeted support without full immobilization. By working with natural movement rather than restricting it, the Relief Patch for Thumb helps users remain active while reducing irritation associated with repetitive thumb motion.
[ To know more about Relief Patch for Thumb: Click Here ]
The Relief Patch for Thumb helps manage tenosynovitis by supporting the thumb and guiding movement to reduce irritation of the tendon sheath. Its 4-way stretch material provides gentle compression and multidirectional support, helping improve joint stability and muscle function during daily activities. The wave-pattern adhesive is designed to slightly lift the skin, which may help enhance local circulation and contribute to pain relief, especially during repetitive thumb use.
The primary difference between a Relief Patch for Thumb and a brace lies in the level of motion control.
Its 4-way stretch material provides gentle compression and multidirectional support, allowing functional thumb movement while helping reduce mechanical stress on irritated tendons. This makes it suitable for:
In contrast, a brace offers more rigid stabilization and consistent restriction of motion. Bracing may be necessary in cases of:
However, prolonged immobilization may limit daily hand use. Therefore, choosing between dynamic support and rigid bracing should depend on symptom severity, functional demands, and professional medical guidance.

The recovery time for tenosynovitis (tendon inflammation) varies widely, ranging from just a few days to several months, depending on the type of condition and the treatment used. Achilles tendon inflammation typically requires 4 to 6 months of therapy without surgery, with about 51% of patients recovering after an average of 18 weeks (E. Johnston et al., 1997). For De Quervain’s tenosynovitis (pain in the thumb side of the wrist), approximately 90% of patients are treated effectively with corticosteroid injections, with some achieving relief very quickly (B. Anderson et al., 1991). Notably, if the symptoms have been present for less than 3 months, the treatment is more likely to be successful (A. R. Golas et al., 2015). Ultimately, healing time depends critically on the specific type of tenosynovitis, how long you have had the symptoms, and the chosen treatment approach.
Yes, doing the right exercises can actually help you recover. For example, researchers developed a specific home strengthening program for De Quervain’s tenosynovitis (Michele Rutkowski et al., 2023). Additionally, a study found that "eccentric" exercises (which lengthen the muscle) can help fully resolve symptoms (Emily R. Howell et al., 2012). However, you must be careful. You cannot just do any exercise. The exercises must be gentle and aimed at reducing inflammation, not aggravating it. The safest approach is to seek professional medical evaluation and exercise guidance to ensure safety.
Tenosynovitis is indeed closely related to aging and degeneration. Evidence suggests it is fundamentally a degenerative process (tissue breakdown) rather than purely an inflammatory condition (C. Arend et al., 2012). Microscopic analysis reveals that the tendon sheath accumulates specific substances, which is a clear sign that the tissue is breaking down. This means tenosynovitis is not only caused by inflammation, but also by gradual tissue breakdown over time. Repeated use without enough rest can create tiny injuries in the tendon, and as these small injuries accumulate, both degeneration and inflammation develop together, leading to pain and stiffness.
You should see a doctor if your symptoms last for more than a few weeks, disrupt your daily life, or do not get better with rest and basic home care. Specifically, seek medical attention if you experience:
Lian Lee, PT, MSc
Licensed physical therapist with 15+ years of rehabilitation experience. Holding an MSc in Biomedical Engineering from Imperial College London and a PT degree from National Yang Ming University, she specializes in clinical biomechanics and the research and development of rehabilitative technologies.
Rex Lin, PT, MHA
Licensed physical therapist with 10+ years of rehabilitation experience. Holding an MHA from Asia University and a PT degree from Chang Gung University, he specializes in biomechanical analysis and the functional application of orthopedic supports.
Founded in Seattle, Washington in 1997, OPPO has grown into a trusted international medical brand serving over 3.5 million users across 60 countries. With a commitment to precision, safety, and innovation, OPPO designs and manufactures more than 550 products and holds over 30 patents recognized by global design awards such as Red Dot and iF. Guided by the belief that everyone deserves the opportunity to live without limitation, OPPO continues to empower people worldwide to move with confidence and comfort.
Copy Link